$149 New Patient Special
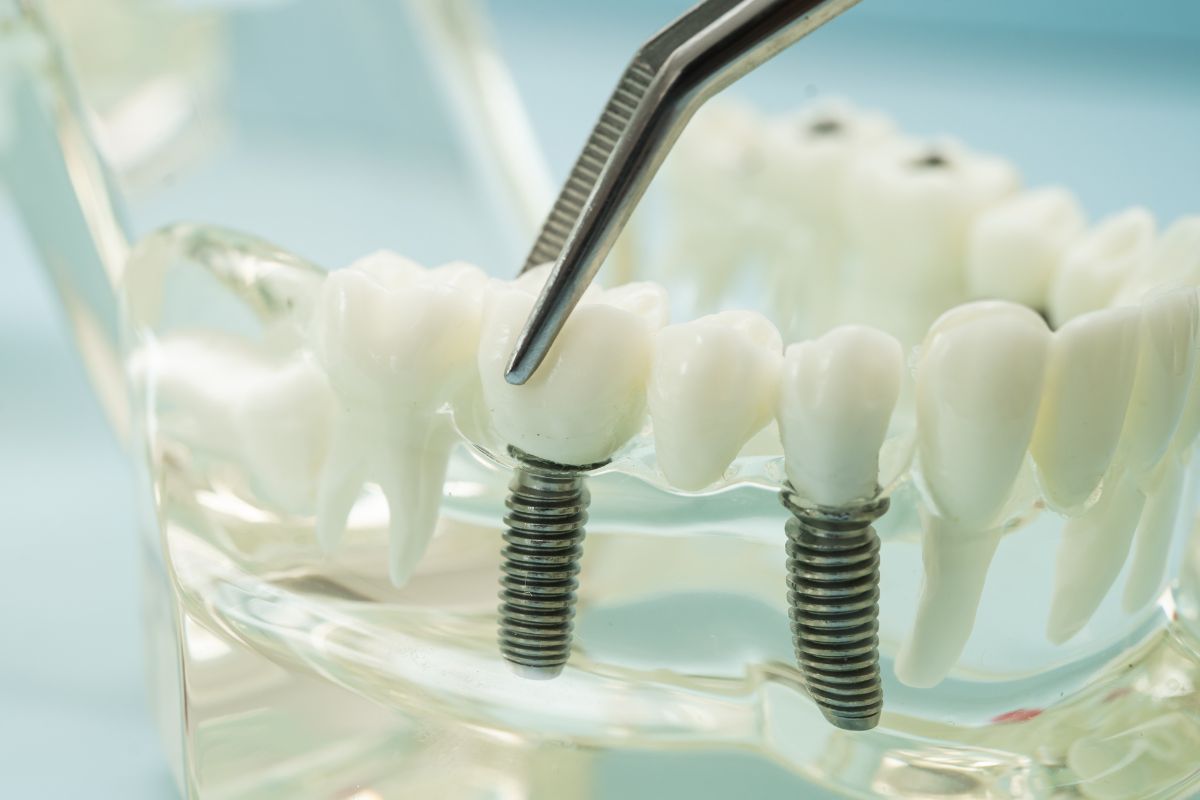
That’s one of the first questions people ask, and it’s the right one. A full-arch restoration is a significant commitment, and you deserve a straight answer rather than vague reassurances. The short version: with proper care and a good candidate match, All-on-4 implants can last decades. Some patients keep their implants for life. But longevity isn’t automatic. It depends on several factors that are genuinely within your control.
Here’s what the research shows, what affects the timeline, and how to make sure you’re getting the most out of your investment.
What the Research Says About Longevity
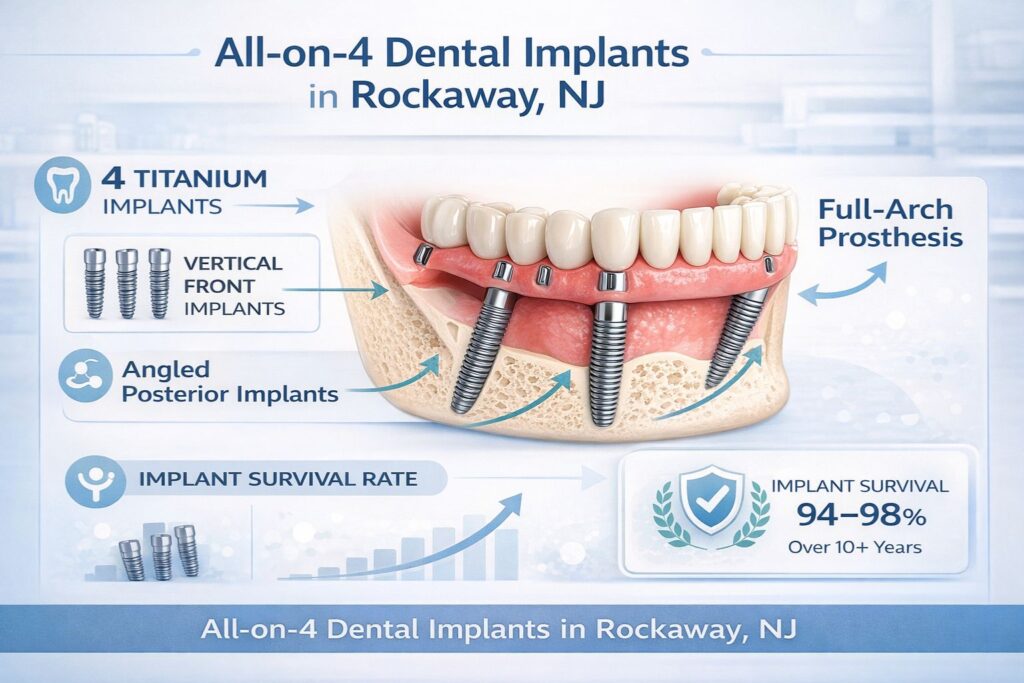
Long-term clinical data on All-on-4 outcomes are encouraging. Studies tracking patients over 10 years report implant survival rates consistently above 94 percent, with many showing rates closer to 98 percent when patients are properly selected and follow post-operative protocols. That’s not marketing language – it’s peer-reviewed data from multiple research groups.
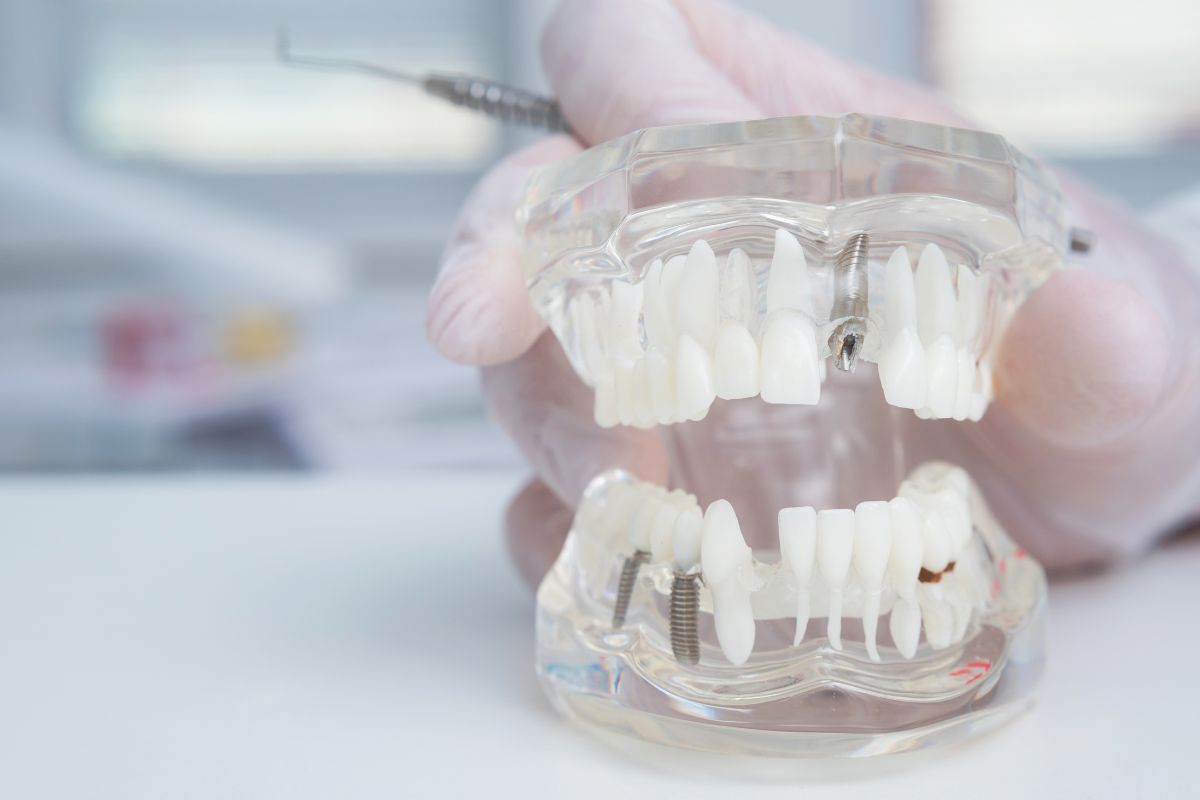
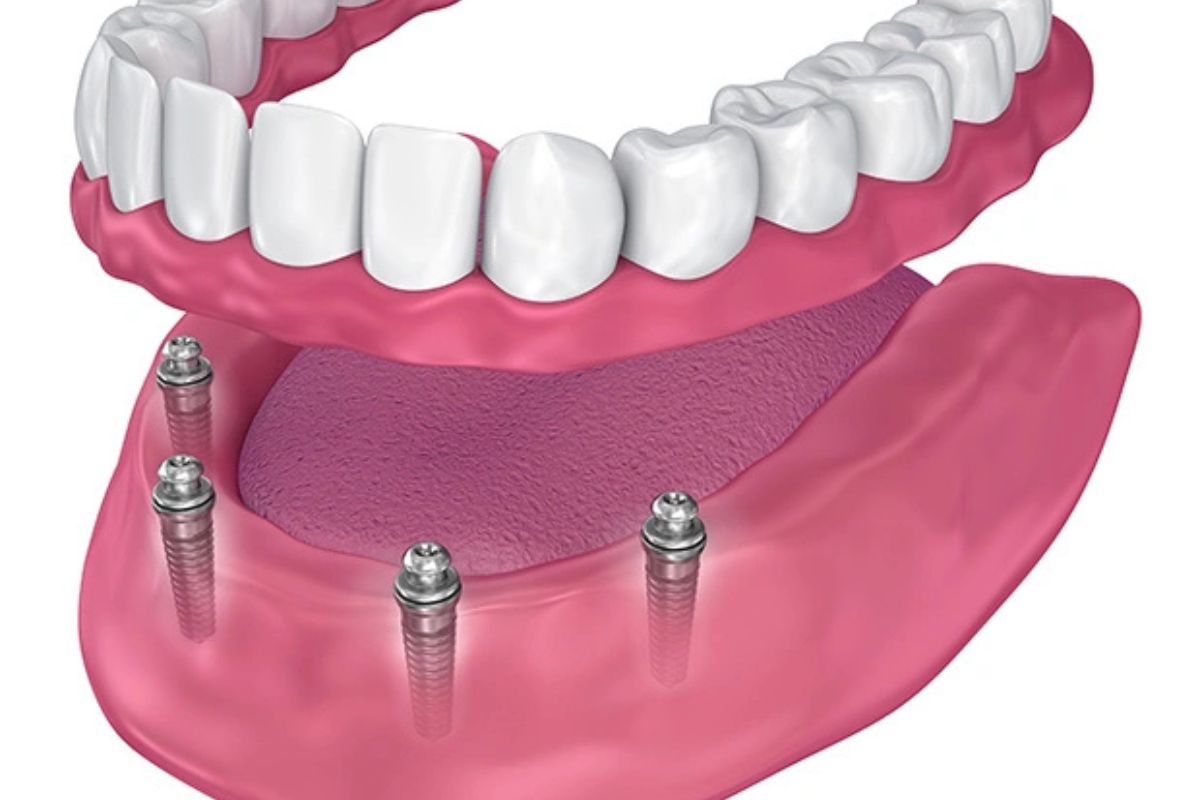
All-on-4 dental implants work by anchoring a full-arch prosthesis to just four titanium posts placed strategically in the jaw. Two implants go in at the front, and two are angled toward the back – this angulation is what allows the procedure to work even in patients with some degree of bone loss, bypassing the need for bone grafting in many cases.
The titanium posts themselves are designed to last a lifetime. What varies more is the prosthesis – the visible arch of teeth attached to those posts. Depending on the material used, the prosthesis may need to be replaced or upgraded after 10 to 20 years of use.
What Affects How Long Your Implants Last
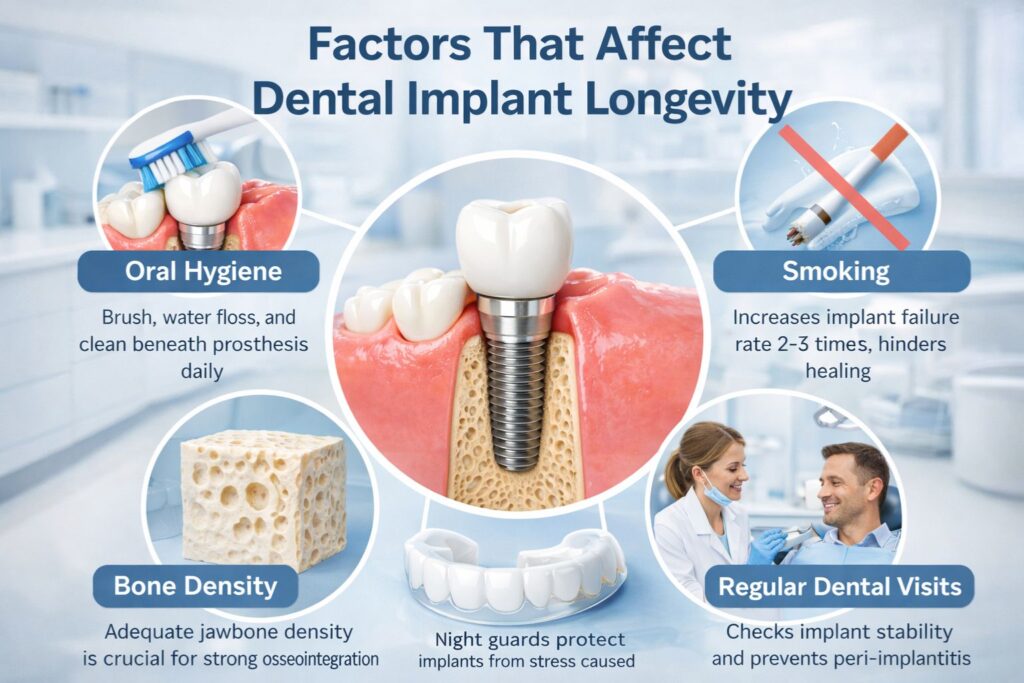
Not all outcomes are equal, and the difference usually comes down to a handful of key variables. Knowing them helps you make informed decisions before and after your procedure.
Your Oral Hygiene Habits
This one carries more weight than most patients expect. Peri-implantitis – an inflammatory condition affecting the tissue and bone around implants is one of the leading causes of implant failure. It’s essentially the implant equivalent of gum disease, and it’s largely preventable. Brushing twice daily, using a water flosser, and consistently cleaning beneath the prosthesis dramatically reduce your risk.
Smoking
If you smoke, your implant failure risk increases. Research has shown that smokers face failure rates two to three times higher than non-smokers. Smoking restricts blood flow, impairs healing, and interferes with osseointegration (the process where the titanium post fuses with your jawbone). Quitting before surgery and staying quit during recovery makes a measurable difference.
Bone Density and Jaw Health
Strong osseointegration requires adequate bone quality. Your provider will assess this before surgery, but maintaining bone density long term matters, too. Regular dental checkups allow your care team to monitor the bone levels around your implants and catch any changes early.
Ongoing Professional Maintenance
Patients who keep their regular dental appointments without fail usually have better long-term outcomes. These visits aren’t just routine cleanings – they’re an opportunity to check implant stability, assess the prosthesis fit, and identify early signs of peri-implant issues before they become serious problems.
Teeth Grinding (Bruxism)
Chronic grinding or clenching puts significant stress on both the implant posts and the prosthesis. If you grind your teeth, your provider may recommend a night guard to protect your restoration. Unmanaged bruxism is one of the more common mechanical reasons prostheses crack or loosen prematurely.
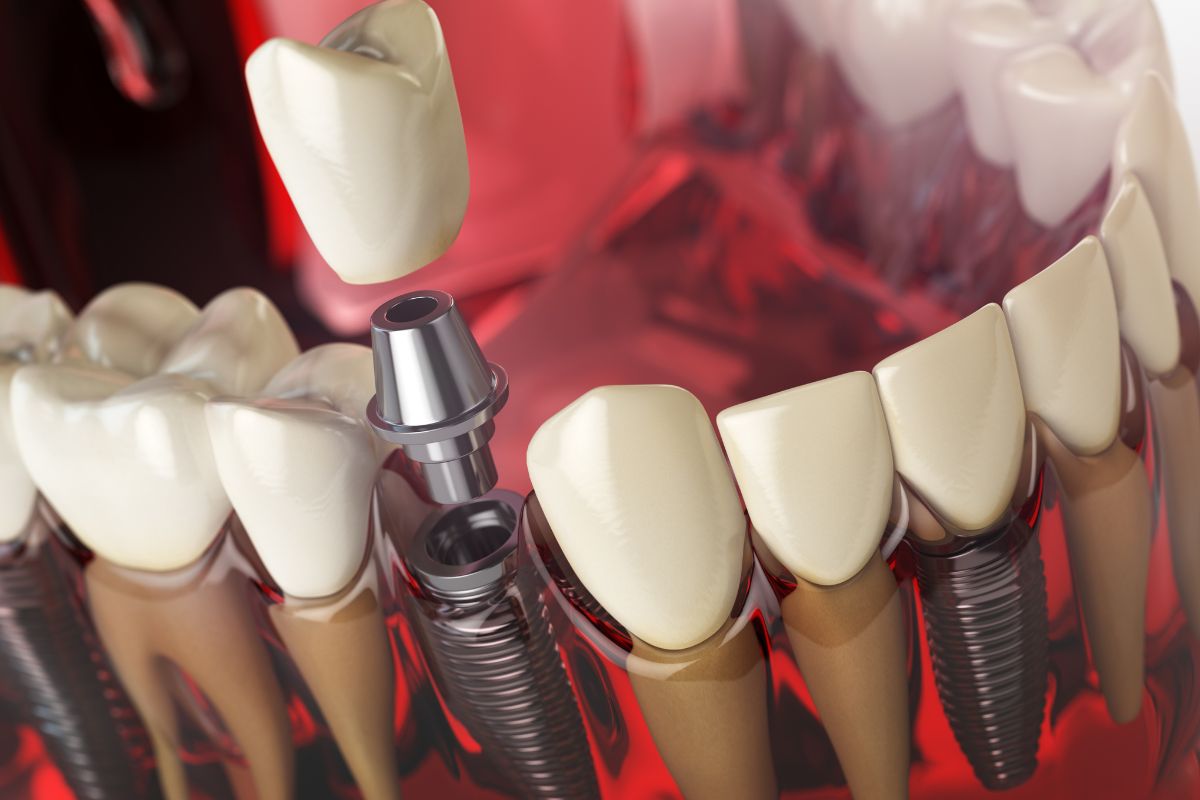
The Difference Between the Implant Post and the Prosthesis
This distinction matters when thinking about long-term costs and planning. The titanium implant posts, once fully integrated with the jawbone, are remarkably durable. Barring infection, injury, or significant bone loss, they’re designed to be permanent.
The prosthesis (the actual arch of replacement teeth) has a different lifespan. Acrylic prostheses typically last 5 to 10 years before needing replacement. Zirconia or other higher-grade materials tend to last longer, often 15 to 20 years. Your provider can walk you through which material makes sense based on your budget, bone structure, and lifestyle.
The implant posts can last a lifetime. The prosthesis likely needs attention within the 10- to 20-year range. Your habits between now and then – how consistently you clean, whether you smoke, how often you show up for checkups shape the outcome more than almost any clinical factor.
The patients who do best aren’t necessarily the ones who started with perfect bone density. They’re the ones who stay engaged with their care.
Contact Rockaway Dental Center today and schedule your consultation.
People Also Ask
Yes, though it’s uncommon. Late failures are usually linked to peri-implantitis, unmanaged bruxism, or significant bone loss over time. Regular monitoring helps catch warning signs early. Most long-term failures are preventable with consistent hygiene and professional maintenance appointments.
Most patients describe the sensation as very close to natural teeth. Because the prosthesis is fixed, it provides a stable biting force and doesn’t shift while eating or speaking. Sensation through the implant differs slightly from a natural tooth root, but function is comparable.
The prosthesis may still be supportable depending on which implant is affected and the condition of the others. Your provider will assess the situation and discuss options, which may include replacing the failed post once the area has healed. Not all single-implant issues require full reconstruction.
Most providers recommend checkups every six months, though some patients benefit from more frequent monitoring in the first year post-surgery. These visits assess implant stability, prosthesis fit, and bone levels — all critical for catching problems early.
Yes. Many patients who initially received an acrylic prosthesis choose to upgrade to a higher-grade material at a later stage. Your provider can assess the condition of your implant posts and prosthesis and discuss whether an upgrade makes clinical and practical sense for you.